What Is Low Energy Availability (LEA) and Why It Matters
Tracking, Planning, Eating “Well” — And Still Missing Something
I’ve kept food diaries on and off for years. Every now and then, I’d choose a 2–6 week period to track my meals and macros, just to see what and how I was actually eating. I’ve also meal-prepped for years, and I have a little meal-prep carry-on bag that goes with me pretty much everywhere — I’m always bringing my own food, I’m used to it.
I want to say I mostly ate intuitively, but that’s not entirely true.
I never counted calories or macros, I just followed my beliefs and knowledge about what a healthy diet should look like. I know which ingredients are considered healthy, when to eat, and roughly how much. So, in that sense, it felt intuitive.
But if I’m being truly honest, there was also a lot of quiet restriction layered into it, especially around carbohydrates (but more on that later).
When I looked at the data from my food diaries over the years, I could see that my calorie and macro averages were always the same, regardless of the time period tracked. This made sense, since my diet had been pretty much the same for years.
What did fluctuate, though, was my day-to-day intake (this was a clue I now know🫢). Some days were much lower, others higher — but when I zoomed out and looked at longer tracking periods (2–6 weeks), the totals always evened out.
I eat clean and healthy. I choose organic whole foods. I don’t eat dairy, gluten, or refined sugar. My diet consists mostly of lean, clean protein (chicken, beef, eggs, fish, organic tofu), plenty of fruits and veggies, healthy fats (ghee, olive oil, nuts, seeds), and certain carbs — mostly lower-GI (Glycemic Index) ones like quinoa, hummus, and oats for example.
I know how to build a balanced plate. I even try to follow Ayurvedic principles — soaking nuts and seeds, being mindful of digestion, avoiding foods I believed would irritate my gut. Basically, I was doing everything I thought was right: eating clean, being careful, and trying to support my health.
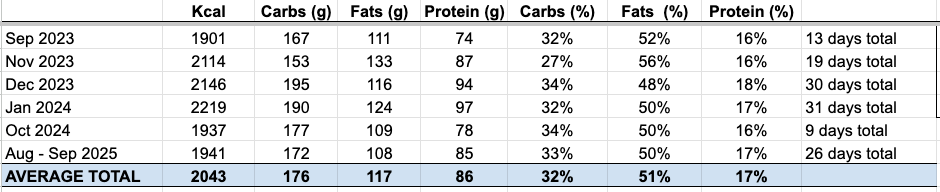
Here’s a screenshot of the total averages from several of those tracked periods over the years:
So, on paper, it looked fine, and I genuinely thought: oh good, I’m eating 2000+ kcal per day on average, surely that’s enough.
Despite many doctors and health professionals telling me for years that I was underweight (which I was, looking at my body composition results), I would always think and say: well, what can I do? I’m eating enough! Look! (pointing at the tracked info in my spreadsheets).
But as per my recent findings, it turns out I’ve been unintentionally underfueling myself for years!
I had no idea!
The Invisible Deficit: Low Energy Availability
There’s this measure called energy availability, or EA. EA is not about calories eaten, but how much energy is left for your body after training and daily movement.
EA = energy eaten − energy used for exercise.
What’s left is the energy your body has available to run everything else.
You can eat “enough” calories, you can even eat “healthy,” and still be chronically underfueled — especially as a woman. That was the case for me. And when that happens, the body enters a state called low energy availability, or LEA.
By definition, LEA occurs when the energy you consume is not sufficient to support both your exercise demands and your basic physiological functions. In other words, you’re not eating enough to support both your training and your basic biological needs.
One of the clearest ways I’ve heard low energy availability explained comes from Dr. Katie Schofield, a doctorate specializing in LEA. She compares it to a phone going into low battery mode:
“It still functions, but the screen goes dim, and some of the apps start shutting down to conserve energy. Only in the case of your body, those “apps” are your organ systems, like your reproductive and endocrine systems!” — ROAR
What struck me most when reading ROAR was how common this actually is. According to the research Dr. Stacy Sims references, low energy availability isn’t rare or extreme — it’s something clinicians see every day.
Some women end up in this state because they’ve been restricting food for years (maybe most of their lives) and they are afraid to eat enough.
Others can fall into it unintentionally when they increase training intensity or volume, but don’t register that they need to eat more.
“So many women barely achieve their resting metabolic rate needs (about 1,300 to 1,400 kilocalories)—the amount of calories needed to just lie on the couch watching Netflix, let alone eat enough for life and training.
As an active woman, you need to eat enough, being sure to consume a well-rounded diet that includes ample amounts of fruits and vegetables and all your macronutrients (protein, fats, and carbohydrates). For most active women, that’s well north of 2,000 calories a day. In fact, the range is often 2,300 to 4,000 calories depending on the sport, training block, and body composition.” — Dr. Stacy Sims, ROAR
Why “Calories In” ≠ Energy Available
Low energy availability does not always mean “eating too few calories.” This is an important distinction to make. You can be eating what looks like a reasonable amount of food — even hitting a decent daily calorie number — and still be in an energy deficit at the physiological level.
LEA can come from several places, not just low intake. It can happen when:
You’re not eating enough for what your body actually needs, especially once exercise is added in
You’re training more or harder than you’re fueling for
Carbohydrates are too low, which can signal a lack of safety to the brain and liver (this was another clue for me!)
You go too long without eating, leaving your body in catch-up mode
Sleep is poor, which raises stress hormones and increases energy demand
Life stress is high, even if food intake hasn’t changed
This is why energy availability can be so misleading — your body can be at a “normal” weight, look lean, fit, or even strong, and still be operating in an energy deficit internally.
What Does Low Energy Availability (LEA) Look Like in the Body
Low energy availability doesn’t show up as one single symptom. It shows up as a pattern — a collection of signals that the body doesn’t have enough fuel left over to fully support all of its systems.
When energy availability drops, the body starts prioritizing survival. Systems that are not essential in the short term begin to downshift, conserve, or shut down altogether.
Some of the most common signs include:
Performance and recovery changes
Training starts to feel harder, even though you’re doing “everything right.” Strength, power, or endurance may plateau or decline. Heart rate can feel off, recovery takes longer, and workouts stop producing the results you expect.
Menstrual and hormonal disruptions
For women, changes in the menstrual cycle are one of the clearest red flags. Periods may become lighter or shorter, arrive irregularly, or disappear altogether. This is a signal that the body doesn’t perceive enough energy coming in to support reproductive and hormone health.
Bone health decline
Low energy availability interferes with bone remodeling. Over time, this can increase the risk of stress reactions, stress fractures, and bone density loss — often before performance noticeably drops.
Lowered immunity
Frequent colds, infections, or slower healing can appear as the immune system no longer has sufficient resources to function optimally.
Digestive issues
LEA can disrupt gut function and the microbiome. Symptoms may include bloating, gas, constipation or diarrhea, nausea, or feeling generally unwell after eating — even when the food itself is “clean” or familiar.
Cognitive and coordination changes
Fatigue affects more than muscles. Reaction time, coordination, focus, and mental sharpness can decline when the brain isn’t adequately fueled.
Mood shifts and chronic irritability
Low energy availability often shows up emotionally as irritability, anxiety, low mood, or a sense of being constantly on edge. Hunger cues can become unreliable — some people feel flat and disconnected from hunger, while others experience sudden waves of hunger at odd times, like late at night or while running errands.
Why Energy Availability Matters — Especially for Women
Over the last years, certain diet trends have become very popular, especially in fitness, endurance sports, and wellness spaces. Many of them revolve around the same idea:
eat fewer carbs and rely more on fat and protein for fuel.
These approaches show up under different names — low-carb, high-fat, keto, paleo, metabolic efficiency, intermittent fasting — but the core message is similar: reduce carbs, increase fat and protein, and often eat less or less often. And for many people, these approaches seem to work very well.
But here’s the key part I didn’t understand for a long time: women do not respond to these strategies the same way men do.
When women go too low in carbs, the brain can interpret it as a sign that food isn’t reliably available. Basically, the body thinks: we don’t have enough coming in to comfortably run everything — let alone carry a pregnancy. So it pulls back on hormone production. Signals for ovulation and estrogen (especially estradiol) can drop, while stress hormones like cortisol rise.
From a survival viewpoint, it makes sense. When the body senses food scarcity, the priority becomes getting through the day — not creating new life.
Men, however, tend to respond differently. In men, a low-carb state can signal the body to become more “fight-ready”: leaning up, maintaining or increasing testosterone, and becoming more physically driven.
As Dr. Stacy Sims explains:
“This alteration in reproductive hormones is why so many women struggle on intermittent fasting, keto, and low-carb, high-fat diets while men tend to thrive on them. Women are not small men. Keep this in mind before jumping onto the latest diet bandwagon.” — Dr. Stacy Sims, ROAR
What Low Energy Availability (LEA) Looked Like in My Body
For me, low energy availability wasn’t dramatic or obvious at first. It was subtle, gradual, and confusing.
It looked like this:
Constant fatigue — even though I was eating “healthy”
Ongoing digestive issues and IBS symptoms
Mood disorders (feeling low, unmotivated, depressed)
Cravings and crashes later in the day
A nervous system that felt fragile instead of resilient
Feeling weak, getting tired quickly when exercising
Cognitive decline (not being able to focus or concentrate, feeling like my brain wasn’t working anymore)
Poor sleep
A missing menstrual cycle
And eventually, an osteoporosis diagnosis at the age of 40
I’d been having these symptoms for years. For years!!!
I went to dozens of health professionals — the gut doctor, the hormone doctor, the gynecologist, alternative therapy experts, psychologists, you name it — asking:
What’s wrong with my gut and digestion?
Why does everything I eat seem to hurt me even though I’m super healthy?
Why is my brain no longer working?
Why am I not sleeping anymore?
Why can I only walk, swim, or bike for a short time before I’m completely wiped out for the rest of the day?
Where did my period go, and why isn’t it coming back?
Why am I always so tired?
Why do I feel so low, unmotivated, depressed?
Why am I so sensitive that I can’t handle crowded places for long and just want to be alone all the time?
I could not figure it out!
Most of the tests always came back “normal.” No obvious disease. No major diagnosis. But then why was I feeling so off every single day?
It was like a mystery. I just could not get it. I was in my 30s, for God’s sake! Aren’t I too young for all this shit?,I kept thinking.
Then I read ROAR, and it all clicked: the energy availability, the low-carb, high-fat diet, the missing cycle, the fatigue, the mood shifts, the gut issues. It wasn’t ten separate problems, it was one root issue showing up in many ways.
Nothing wrong with my endocrine system — just not getting the signals it needed.
Nothing wrong with my gut — just microbiome and stress-related.
Nothing wrong with my brain — it just needed proper fuel, for God’s sake!
And on it goes.
My body simply wasn’t getting the consistent, sufficient energy it needed — especially carbohydrates — to feel safe and function properly.
Recently, I went for a bone density scan. It came back with an osteoporosis diagnosis. I’m only 40 years old..
Not because of a rare disease, not because of some unknown illness (which I am incredibly grateful for), but likely as a result of years of underfueling and hormonal suppression.
That’s not something to take lightly.
As Dr. Stacy Sims explains:
“One of the downstream consequences of disrupting your hormones with LEA is serious and potentially lasting negative impacts on your skeletal system. Without enough energy, your osteoblasts (the cells that build bone) and osteoclasts (the cells that break down and resorb bone) can’t do their job properly, and you end up breaking down more than you build up.” — ROAR
For me, this wasn’t theoretical anymore. It was real.
The EA Mistake I Made (and How Carbs Kept Being the Missing Piece)
My low energy availability didn’t come from one dramatic mistake, but from a pattern. A pattern that, on the surface, looked disciplined, clean, healthy, “optimized.” But underneath, it was quietly underfueling me.
1. High fat, low carb eating
I was eating plenty of fat, and fat is calorie-dense. But calories are not the same as usable energy.
Fat converts more slowly, and my body — especially with training, cold exposure, hiking, and daily stress — needed glucose. It needed readily available fuel.
So even when my total calories looked “okay,” my available energy wasn’t. It was like I was telling my body: here’s energy… just not in the form you need right now.
2. Long gaps and unstable timing
I was fasting in the mornings, training before fueling, and waiting hours before eating after I woke up. I was eating three meals a day, sometimes with long stretches in between (4-5 hours vs 3 hours).
Energy availability isn’t just about how much you eat, it’s also about when energy arrives. So, when meals are delayed and gaps are long, the body leans more on stress hormones — cortisol and adrenaline — to keep you going. That works… for a while. But later in the day, it often shows up as crashes, cravings, irritability, or feeling wired and tired.
3. “Clean eating” that was too light
I was eating lots of vegetables, clean protein, and healthy fats, but carbs were low, often delayed, and sometimes even avoided out of fear. The result? The body stayed in energy conservation mode, and hormones, cycle, mood, and recovery paid the price.
It wasn’t that I wasn’t eating. It was that I wasn’t eating in a way that matched my physiology, training load, and nervous system needs.
4. Day to day fluctuations
Remember when I said earlier that when I looked at my average macros, they were always the same — but when I looked at the day-to-day numbers, they fluctuated a lot? That was a clue, I now know.
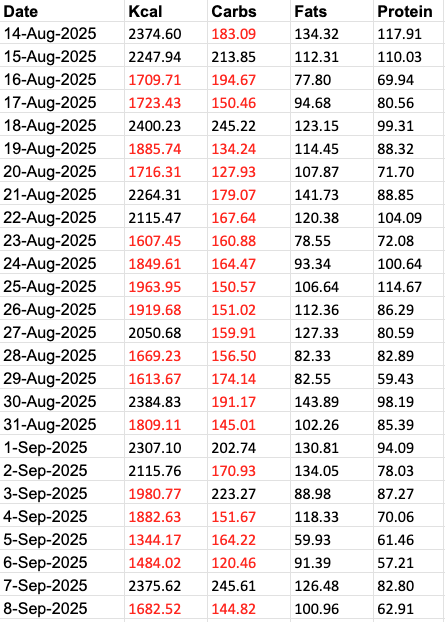
When I looked at my 26-day data more closely, day by day, this is what I saw:
Daily kcal range:
Min: 1,344 kcal
Max: 2,400 kcal
Days below 2,000 kcal: 16 out of 26
Days below 1,800 kcal: 9 out of 26
So, even though my weekly averages looked “fine,” more than 60% of my days were below 2,000 kcal, and over one-third dropped below 1,800.
That kind of fluctuation matters — especially when training and life stress are layered on top.
Carbohydrates told an even clearer story:
Days below 200 g of carbs: 21 out of 26
Days below 160 g of carbs: 11 out of 26
That means roughly 80% of my days were below 200 g of carbs, and almost half were below 160 g. For many active women, that’s already on the low side — especially when combined with training, long meal gaps, and stress.
The pattern
My LEA didn’t come from “not eating enough”, it came from eating in a way that didn’t match my body. On paper, my averages looked good, but in real life, my hormones were wrecked, my nervous system was fragile, and my energy was unstable.
To be completely honest, at some point I had picked up the belief that carbs are bad.
I believed that all carbs are basically sugar — and sugar is bad. That they feed bad bacteria in your gut, cause blood sugar crashes, and will make me fat. I truly believed I was better off without them.
All of this was stuff I had picked up from various health and nutrition professionals I follow. And their advice isn’t necessarily wrong, but it’s always subject to context — in what cases, for whom, and for how long it’s true.
Nutrition is one of the most confusing areas out there. Almost every professional seems to offer new information and advice that contradicts someone else’s. We’re all different — different body types, different health states, different goals. So not everything we hear or see online, even if it has worked very well for many people, is necessarily right for us.
I’m now learning that carbohydrates are not the enemy. They are a necessary, foundational part of a healthy diet and lifestyle — especially for active women. However, not all carbs are the same, and quality, quantity, and timing do matter.
I also noticed something else. Most of the people I follow online who talk about health, wellness, biohacking, and performance… are men.
But I am not a man (surprise! 🙃), and I am only now learning just how different women’s physiology is from men’s. Not all advice that works very well for men works — or is even healthy — for women. When I read ROAR, it shifted something fundamental for me. There have been a few books in my life that have had such a significant impact on me, and this is one of them.
“Women are not small men.”
Looking back, I can see that what I was doing may work very well for some people. But it wasn’t working for me — not for my body type, my schedule, my stress load, my training, and not for me as a woman.
And that realization changed everything.
What “Right EA” Means for Me Right Now
Right now, “right EA” for me means consistency, balance, and eating in a way that makes my body feel safe.
It means eating enough — not just on average, but day to day.
It means making sure carbohydrates are present and available — fuel that my body can actually use.
It means eating regularly — five meals per day, roughly every three hours — so my body doesn’t have to rely on stress hormones to bridge long gaps.
It means fueling around movement — eating before training and eating after training.
It means aiming for a minimum of 2,200–2,300 kcal per day, with roughly 40% from carbohydrates, 35% from fats, and 25% from protein. Not obsessively — but intentionally.
It also means strength training twice per week (for starters) to rebuild lean mass and support my bones.
It’s simple, but it’s not easy when I’ve spent years believing the opposite.
I’m only about two months into this shift, I don’t have a ten-year case study to present, but I’m already noticing changes:
Fewer crashes and cravings.
More stable energy throughout the day.
A steadier mood.
More trust in my body.
And I actually feel like I have the power to lift weights now!
I’m reminding myself that this isn’t about perfection, it’s about alignment.
Energy availability isn’t just a sports science concept, it’s a lens. And for me, it was the missing piece.
This post is informed by current research on female physiology, energy availability, and performance, as well as my own lived experience interpreting and applying this work.
Sources:
Sims, S. (2016). ROAR: How to Match Your Food and Fitness to Your Unique Female Physiology for Optimum Performance, Great Health, and a Strong, Lean Body for Life.
Sims, S., & Yeager, S. (2023). Next Level: Your Guide to Kicking Ass, Feeling Great, and Crushing Goals Through Menopause and Beyond.
Schofield, K. L., Thorpe, H., & Sims, S. T. (2021). Low energy availability in female athletes: A review of physiological mechanisms and health outcomes.Sports Medicine.
Mountjoy, M. et al. (2018). IOC consensus statement on Relative Energy Deficiency in Sport (RED-S).British Journal of Sports Medicine.
Resources:
NutriData food diary tool.
JJ Virgin, Making Sense of the Glycemic Index
JJ Virgin, Sugar Impact Scales
JJ Virgin, Eat by the Plate Guide